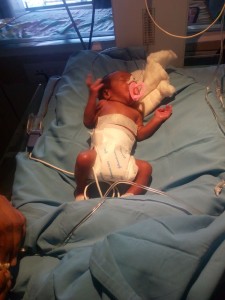
What parents should know about ICU for infants
Birth of a baby is a wonderful but at the same time a very complex process. The baby goes through a profound transition between the life inside the womb and the life outside the womb. Mother and baby both goes through lot of physical and emotional changes.
The baby inside the womb was completely depended on the mother for everything, be it food, nutrition or oxygen. But after the birth the baby must start adjusting to the outside environment and the body starts functioning independently. This adjustment includes correct working of all the systems like digestive, immune, nervous, respiratory etc.
No pregnant women would ever expect her baby to wind up in NICU (Neonatal Intensive Care Unit) after birth but at times some emergency conditions may erupt which makes the admission compulsory for the baby’s survival or healthy future.
I had an in length discussion with my Neonatologist and pediarican husband, Dr. Haresh (M.D Pediatrics). With the help of his 10 years of experience and expertise in New born care ( 4 yrs with Sterling Hospital NICU and 6 yrs at his own set up -Gujarat Child Care Hospital), here I list down the 5 most common reasons for admission in NICU:
1. Preterm Birth:
Preterm is defined as any baby born alive before completion of 37th week of pregnancy. Also there is sub category of premature births as per the gestational age:
- Extremely Premature (<28 weeks)
- Very Premature (<32 weeks)
- Moderate to late Preterm (32 to <37 weeks)
Any births through induction or surgery before the completion of 39th week should be strictly avoided unless medically needed.
According to the latest WHO research (November ‘2015), globally India ranks first with the greatest number of Preterm Births.
“As per World Health Organisation (WHO) Publication ‘Born too Soon: The Global Action Report on Preterm Birth’ out of an estimated annual 2.7 crore live births, in India 35 lakh babies are born preterm and out of these 3.03 lakh babies die due to complication of preterm birth,” the Minister said while replying to a question in Rajya Sabha.
The problem:
Globally, prematurity is the leading cause of death in children under the age of 5. And in almost all countries with reliable data, preterm birth rates are increasing.
Inequalities in survival rates around the world are stark. In low-income settings, half of the babies born at or below 32 weeks (2 months early) die due to a lack of feasible, cost-effective care, such as warmth, breastfeeding support, and basic care for infections and breathing difficulties. In high-income countries, almost all of these babies survive.
The solution:
More than three-quarters of premature babies can be saved with feasible, cost-effective care, e.g. essential care during child birth and in the postnatal period for every mother and baby, antenatal steroid injections (given to pregnant women at risk of preterm labour and under set criteria to strengthen the babies’ lungs), kangaroo mother care (the baby is carried by the mother with skin-to-skin contact and frequent breastfeeding) and antibiotics to treat newborn infections.
2. Jaundice:
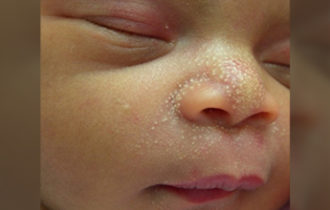
Babies with jaundice have a yellowish color to their skin ( in newborn babies jaundice is to be seen in skin ) and eyes. Jaundice occurs when the liver is too immature or sick to remove a waste product called bilirubin from the blood. Bilirubin is formed when old red blood cells break down. Jaundice is especially common in premature babies, feeding problem babies because of less amount of breast milk and in babies who have blood type incompatibilities with their mothers (such as Rh disease, ABO incompatibility or G6PD disease).
Jaundice itself does not usually cause harm to a baby. But if the bilirubin level gets too high, it can cause more serious problems.like convulsion and cerebral palsy ,which is causing permanent damage in brain and deafness. For this reason, the baby’s bilirubin level is checked frequently. If it gets too high, he is treated with special blue lights (phototherapy) that help the body break down and eliminate bilirubin.
Occasionally, a baby will need a special type of blood transfusion called an exchange transfusion to reduce very high bilirubin levels. In this procedure, some of the baby’s blood is removed and replaced with blood from a donor.
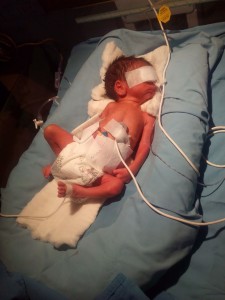 3. Sepsis:
3. Sepsis:
Some babies are admitted to the NICU to determine if they have this potentially dangerous infection of the bloodstream. The infection is caused by a germ which the baby has had difficulty fighting off. Certain lab tests, cultures, and X-rays can help diagnose this condition. These tests may be recommended if your baby has symptoms such as temperature instability, high or low blood sugar levels, breathing problems or low blood pressure. The condition is treated with antibiotics, and the baby is monitored closely for an improvement in symptoms.
The other types of common sepsis are:
- Tummy infection due to offering fresh cow milk to an infant. Fresh cow milk has certain bacteria which can cause severe stomach infection which can be harmful to the baby.
- Infection in mouth which is mostly found in bottle fed babies. Its due to the use of unsterilized bottles or bottles which are not properly sterilized.
4. Respiratory Problems:
Premature babies often have breathing problems because their lungs are not fully developed. Full-term babies also can develop breathing problems due to complications of labor and delivery, birth defects and infections. An infant with breathing problems may be given medicines, a mechanical ventilator to help him breathe, or a combination of these two treatments.
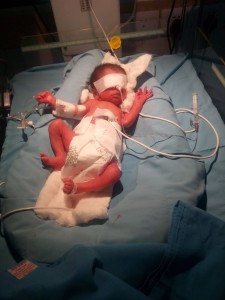 Apnea: Premature babies sometimes do not breathe regularly. A baby may take a long breath, then a short one, then pause for 5 to 10 seconds before starting to breathe normally. This is called periodic breathing. Apnea is when a baby stops breathing for more than 15 seconds. Apnea may be accompanied by a slow heart rate called bradycardia.
Apnea: Premature babies sometimes do not breathe regularly. A baby may take a long breath, then a short one, then pause for 5 to 10 seconds before starting to breathe normally. This is called periodic breathing. Apnea is when a baby stops breathing for more than 15 seconds. Apnea may be accompanied by a slow heart rate called bradycardia.
5. Meconium Aspiration:
Meconium aspiration syndrome occurs when a newborn baby breathes a mixture of meconium and amniotic fluid into the lungs around the time of delivery. It is a serious condition.
Cause:
In some cases, the baby passes meconium while still inside the uterus. This will happen when babies are “under stress” because the supply of blood and oxygen decreases. This is often due to problems with the placenta.
Once the meconium has passed into the surrounding amniotic fluid, the baby may breathe meconium into the lungs. The meconium can also block the infant’s airways right after birth.
This condition is called meconium aspiration. It can cause breathing problems due to swelling (inflammation) in the baby’s lungs after birth.
Treatment:
A special care team should be present when the baby is born if traces of meconium are found in the amniotic fluid. If the baby is active and crying, no treatment is needed.
If the baby is not active and crying right after delivery, a tube is placed in the infant’s airway by a nurse or doctor. Suction is used to remove any meconium. This procedure may be repeated more than once.
If the baby is not breathing or has a low heart rate, the team will help the baby breathe using a face mask attached to a bag that delivers an oxygen mixture to inflate the baby’s lungs.
Other conditions may also include feeding issues, birth defects, heart problems, low blood sugar, keeping warm, pneumonia, anemia etc in which it becomes necessary for the new born to be admitted to the NICU.
Sources :
- http://www.who.int
- https://www.nlm.nih.gov
- http://www.marchofdimes.org